Medical Coding AI Companies: A Guide for Revenue Cycle Leaders


If you've worked in the revenue cycle for any length of time, you've watched the same problems get worse year after year. Median operating margins hovered around 1% through 2025. Denial rates keep climbing as payers analyze claims with closer and closer scrutiny, often using AI tools to deny reimbursement.
The medical coding function sits at the center of it all, and right now, it’s under serious strain. Patient chart volume is so high in many care settings that coders can’t keep up, and many providers end up coding their own charts without oversight.
Coding bottlenecks and errors create a cycle in which claims stall, denials pile up, people burn out, and revenue recognition drags. For years, health systems and physician groups have tried to solve this with more headcount or by outsourcing coding, but that’s not getting the job done. If you work in the revenue cycle, you already know this pain.
The best medical coding AI companies have made something better possible. These platforms use generative AI to code the majority of charts without human intervention, producing faster, more accurate claims while freeing up staff for higher-value work.
Why Traditional Coding Models Fall Short?
Manual coding was sufficient when patient volumes were lower and margins weren’t quite so small. That’s no longer the case.
Here’s a quick peek into what health systems and physician groups are dealing with now:
- Coder shortages that aren’t going away. Thirty-four percent of medical groups say that coders are the most difficult role to hire for in the revenue cycle.
- Limited coder capacity. In ambulatory care settings, patient volumes are so high that professional coders can only process about 30% of charts, according to internal data.
- High denial rates. Initial denials now hover around 15%, according to survey data, and fighting those denials costs an average of $57.23 per claim.
- Slow collections. A/R cycles often stretch for months as coding backlogs and denials delay payment.
Computer-assisted coding (CAC) tools have been around since the 1990s, and for a while, they looked like the answer. But clearly, they’re not. Most CAC systems are built on rules-based logic and aren’t good at reading providers' unstructured clinical notes.
CAC tools aren’t capable of showing why they picked a specific code, so there’s no transparency or audit trail. They suggest codes that then have to be reviewed by a coder, which doesn’t solve the capacity issue at all.
Relying on CAC leaves you in a position where your medical coding workflow can’t scale with chart volume.
The Rise of AI Medical Coding Companies
So what’s different about medical coding AI companies compared to the CAC tools that have been around for decades?
The biggest difference is that technological advances in generative AI (GenAI) and large language models (LLMs) have made true autonomous medical coding possible.
GenAI-native solutions like Arintra can interpret clinical documentation like a human coder, apply payer-specific logic, and assign codes to the majority of charts without human oversight. Only the exceptions get routed to a human coder, and even those have specific suggestions about what needs more work.
Here’s how they compare:
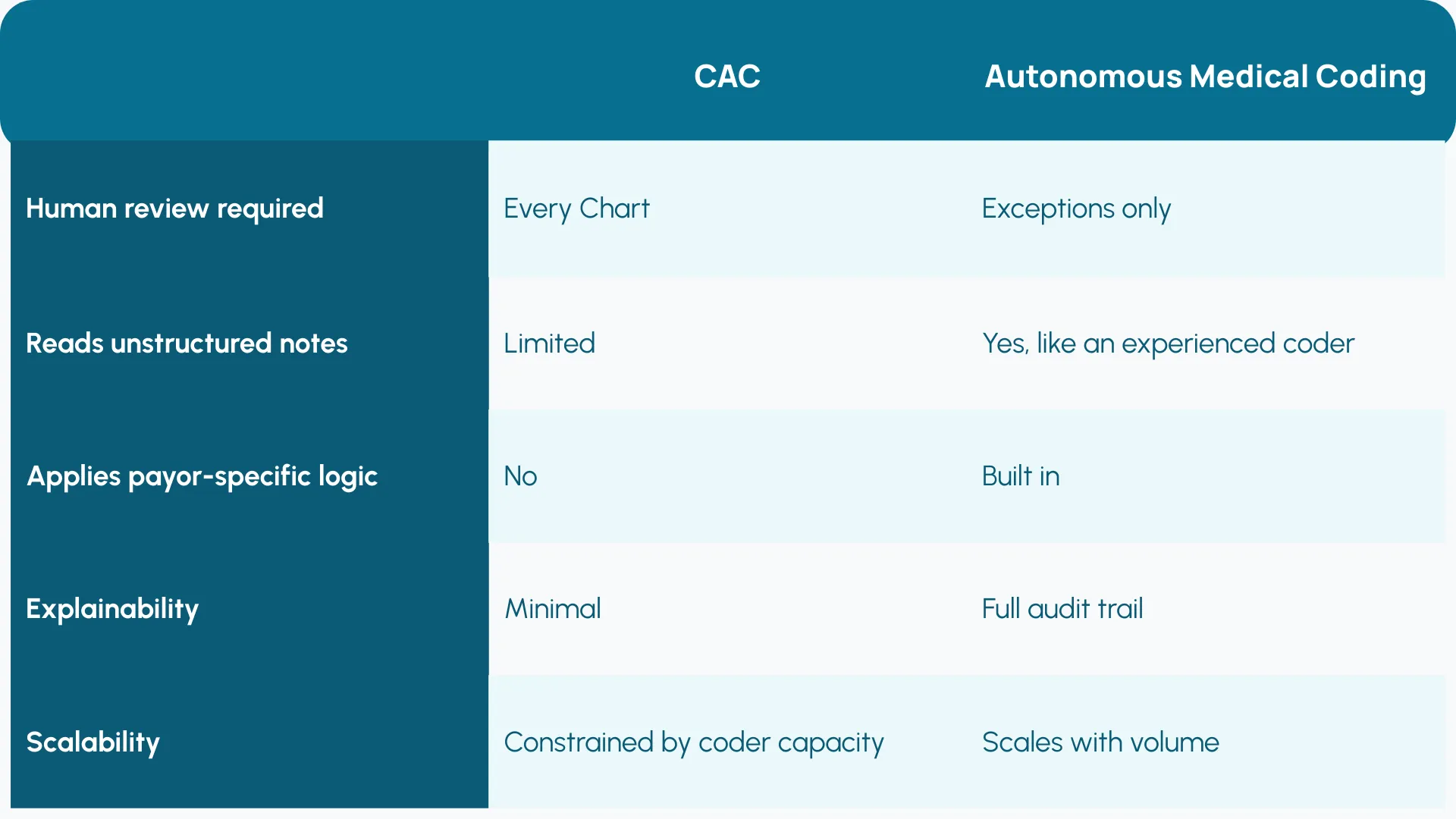
It’s a different model entirely, not just a faster version of CAC. More efficient, yes. But also more transparent, more compliant, and able to scale with your patient volume.
How Do Leading AI Medical Coding Platforms Work?
So how do these platforms actually function? Here's what's under the hood:
Native EHR integration. The best platforms work inside Epic, Athena, or whatever system your providers already use. Coding happens in the background without requiring anyone to change how they document or switch between applications.
Explainable AI. We covered this already, but it’s worth repeating that every coding decision should include reasoning tied to specific documentation. When a payer challenges a claim, the rationale is already there.
Multi-specialty coverage. Ambulatory coding spans dozens of specialties, each with its own complexity. These platforms handle primary care, cardiology, orthopedics, and beyond without requiring a rebuild for each service line.
Continuous learning. Payer rules change constantly. The platform updates automatically as guidelines shift and improves its accuracy over time based on feedback and outcomes.
Real Impact from AI Medical Coding Companies
Numbers are helpful here. Let's look at what medical coding automation has actually done for a few organizations.
Mercyhealth is a multi-regional health system processing over 130,000 claims per month. After deploying autonomous coding, they had:
- 5.1% revenue uplift
- 50% reduction in work queue aging
- 88% of charts go directly to billing without human review
A Midwest health system expanded autonomous coding from primary care into radiology and other specialties. By doing so, they gained:
- 9.2% revenue uplift across service lines
- 96% coding accuracy
- Compliance improvements validated by external auditors
Across Arintra's customer base, the patterns hold:
- 43% reduction in denials
- 12% drop in A/R days
- 32% cost savings in coding operations
This is the kind of impact that's possible today, not years from now.
What Separates the Best AI Medical Coding Companies?
Although relatively new, autonomous coding is changing quickly and expanding into a broader area, which we call revenue assurance. Coding is the foundation, but documentation gaps and payer rules still slow reimbursement. The platforms worth looking at address all of that together.
So if you're evaluating medical coding AI companies, here's where to focus:
Does it go deeper than coding? Look for platforms that also include CDI feedback and payer logic. Coding is the starting place, but it's not the whole picture.
Is it GenAI-native or retrofitted? A lot of vendors are layering AI onto older CAC systems and calling it autonomous. That's not the same thing. Ask whether the platform was built from the ground up on generative AI.
Is there documented ROI? Ask for specifics. What revenue uplift have customers seen? What happened to their denial rates? If a vendor can't point to measured outcomes like 5%+ revenue uplift or 40%+ fewer denials, that tells you something.
These questions will tell you pretty quickly whether a platform is built for the future of medical coding or simply retrofitting the past.
The Competitive Edge of Autonomous Coding
Health systems that get coding right collect more revenue with fewer resources. That's really what this comes down to.
Medical coding AI companies like Arintra are helping organizations get there through faster reimbursement, fewer denials, and coding staff freed up for work that requires their expertise. If you’re curious about what autonomous coding can do for your organization, that’s worth a conversation.
Ready to see how autonomous coding fits into your revenue cycle? Book a demo with Arintra.












